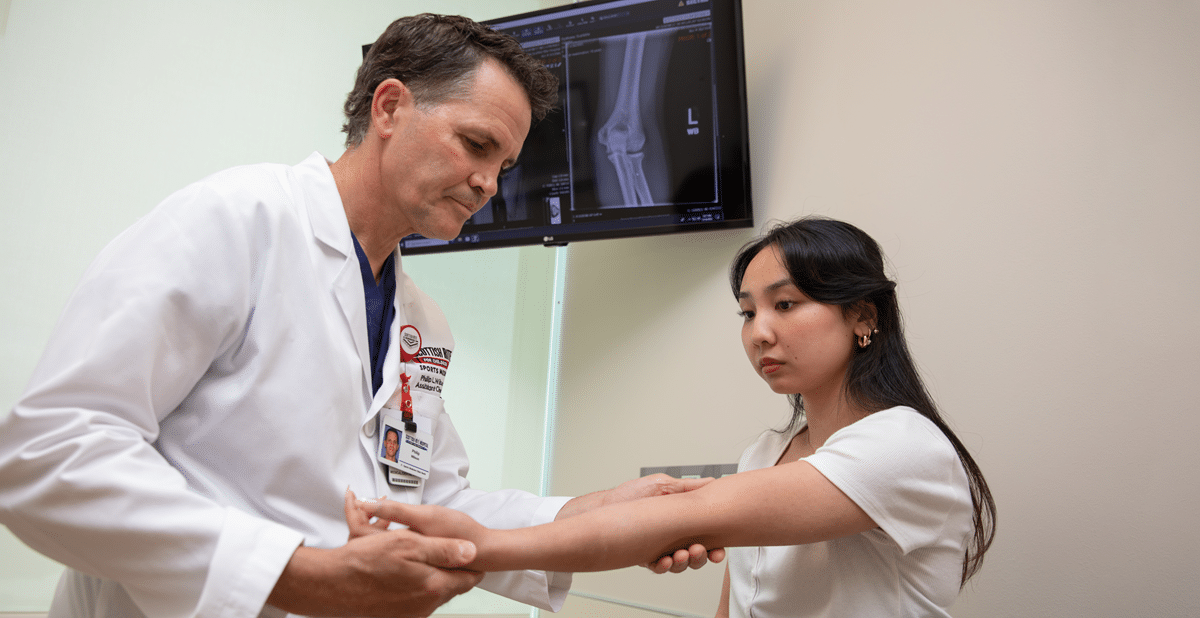
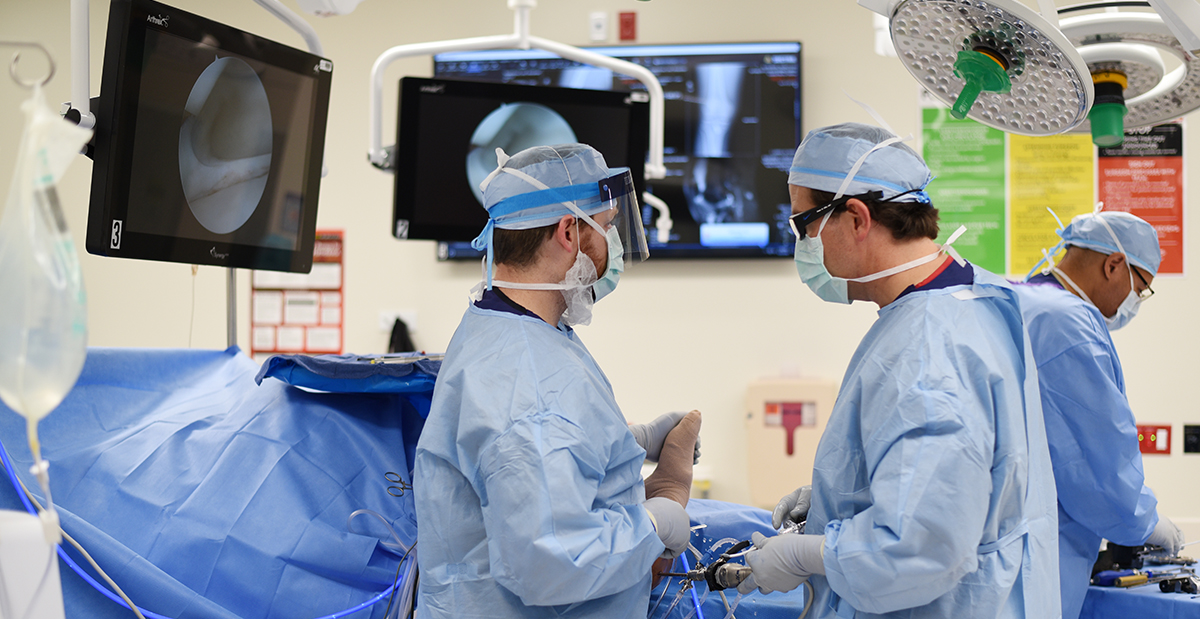
Kamryn spends most of her time on the volleyball court, a sport she has loved since high school. She makes an impact at the net as a server for her college’s volleyball team. The talented 19-year-old was recently recognized as an all-conference player, an honor voted...