If surgery or an orthopedic condition is making it hard for your child to breathe, respiratory therapy can help.
What is Respiratory Therapy?
Respiratory therapy is a series of treatments designed to support your child’s breathing, lung function and oxygen levels.
Your child may need respiratory therapy before or after surgery or to help address breathing issues related to certain orthopedic conditions.
Respiratory therapy is common before surgery and is usually temporary during recovery. It helps your child recover when their breathing is most vulnerable.
Our Approach to Respiratory Therapy
The goal of respiratory therapy is to keep your child’s lungs open and breathing muscles working properly. This proactive approach to care helps protect your child’s lungs, and it can prevent breathing problems before they start.
We typically recommend respiratory therapy for kids and teens:
- Before surgery to assess their lung function and help them prepare for anesthesia and surgery
- After surgery when anesthesia, pain and limited movement can make breathing shallower and more difficult
- During a hospital stay if your child already uses a CPAP or BiPAP machine at home.
- If they have an orthopedic condition that limits their ability to expand their lungs or weakens breathing muscles
Our Respiratory Therapy team work closely with your child’s surgeons, anesthesiologists and nurses. This team-based approach helps ensure breathing support is timed and adjusted to your child’s needs.
Caring for Kids
Your child may be scared or anxious about respiratory therapy. Scottish Rite’s Respiratory Therapy team is here to help your child feel comfortable, confident and informed throughout their treatment. To do this, a pediatric respiratory therapist will explain why each treatment matters and what it will feel like.
Types of Respiratory Therapy
Depending on your child’s needs, their care team will recommend the right type of respiratory therapy treatment for their needs. This may include:
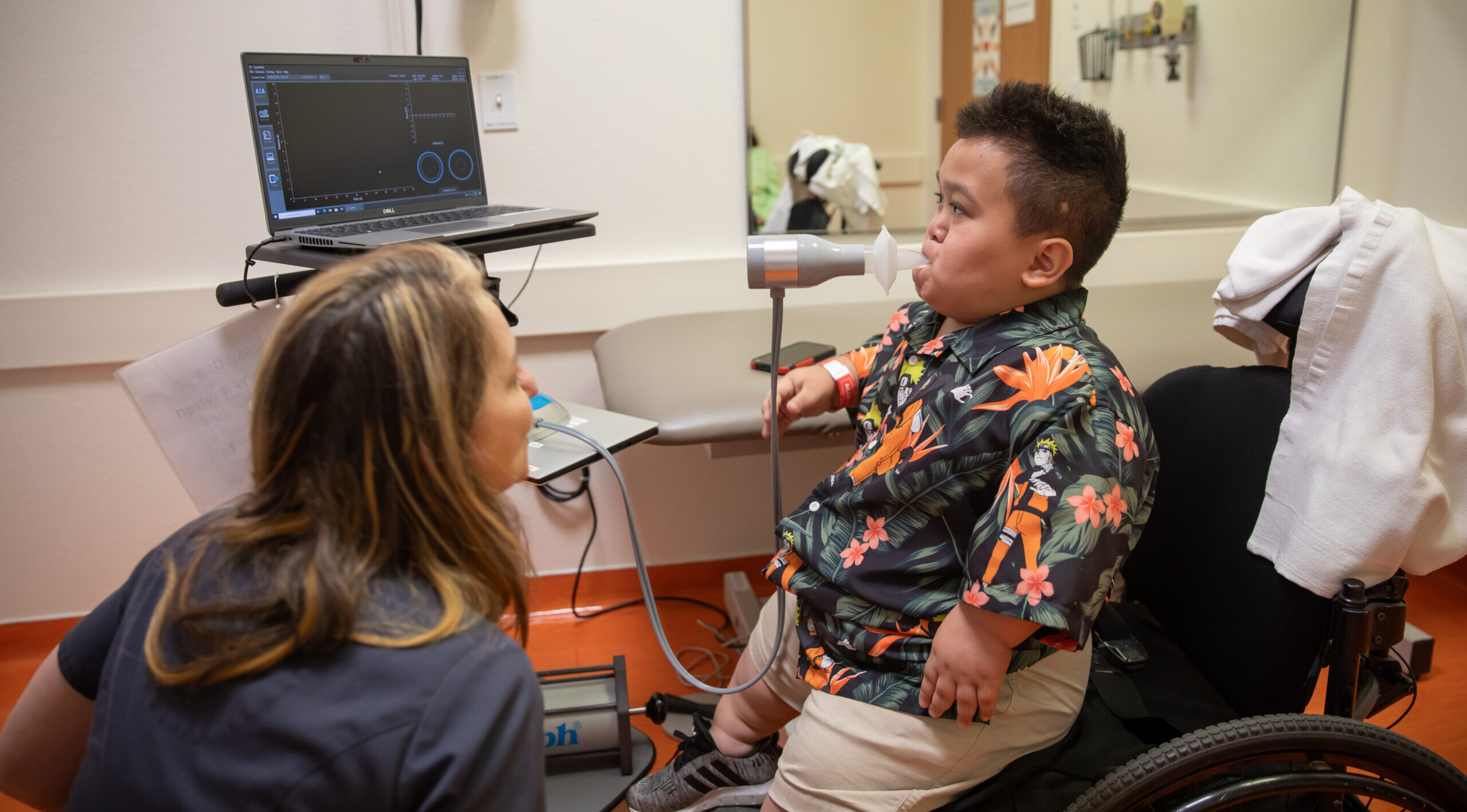
- Incentive spirometry: Breathing exercises that help your child take slow, deep breaths to expand the lungs and prevent complications
- Oxygen therapy: Short-term oxygen support delivered through a mask or nasal cannula for early recovery
- CPAP or BiPAP: Continued use of your child’s home breathing device while staying overnight in the hospital
- Nebulizer treatments: Medications delivered as a mist that support your child’s airways
- Pulmonary function testing: Tests that measure your child’s lung strength and capacity at different stages of their care and recovery
- Ventilator support: Advanced breathing support if your child temporarily cannot breathe on their own
Benefits of Respiratory Therapy
Respiratory therapy offers many benefits, including:
- Improved lung function when your child is most vulnerable, such as after surgery or during an illness
- Reduced risk of lung-related complications, like pneumonia or a collapsed lung
- Safer recovery after anesthesia
- Improved oxygen delivery, which supports healing
- Supports long-term lung health
What to Expect During Respiratory Therapy
Our respiratory therapy team will guide you and your child through each step of treatment.
Before Surgery Consultation
Before surgery, you may meet with a respiratory therapist for a consultation that may include:
- A discussion about your child’s home routine, if applicable
- An overview of respiratory therapy equipment and treatments
- Pulmonary function testing
- What breathing support may look and feel like after surgery
Immediately After Surgery
We will start respiratory therapy as soon as your child wakes up after surgery. This may include:
- Breathing exercises to help your child take slow, deep breaths and expand their lungs
- Temporary oxygen support through a mask or nasal cannula to increase their oxygen levels
Your child’s respiratory therapist will check in regularly and adjust treatment based on your child’s needs throughout the day and night.
We know rest is important after surgery. These regular breathing exercises help prevent complications and help improve your child’s recovery, even while they rest between treatments.
During Recovery
As your child heals, their respiratory therapist adjusts treatment as they progress. Support may include:
- Continuing to follow your child’s home routine with a CPAP, BiPAP or breathing treatments, when possible
- Additional temporary oxygen or other therapies as needed
Our goal is to help your child return to their baseline, which is how they normally breathe before surgery.
Before Leaving the Hospital
Before discharge, your child’s respiratory therapist makes sure your child:
- Has returned to their baseline breathing
- Is back on their home settings for their breathing unit, if used (CPAP/BIPAP)
- Can breathe comfortably without support
- Can maintain healthy oxygen levels
- Can cough effectively
Risks of Respiratory Therapy
There are very few risks associated with respiratory therapy. Our Respiratory Therapy team closely monitor your child’s treatment throughout their care.
Some children feel tired or uncomfortable when they first begin respiratory therapy exercises. Our Respiratory Therapy team can adjust the therapy plan and approach based on your child’s comfort and your preferences.
Why Choose Us?
Orthopedic-focused expertise: Our Respiratory Therapy team have extensive experience supporting children after complex orthopedic and spine surgeries, when breathing risks are highest. They know how to reduce anxiety, explain care clearly and support recovery safely.
Close monitoring and support: Our Respiratory Therapy team is available in the hospital 24/7 to monitor breathing, adjust support and respond quickly if your child’s needs change. If your child is hospitalized, you can feel confident they are receiving expert breathing support and care at every stage of recovery.